 Friday, Aug 18
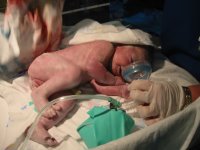
Friday, Aug 18Kaitlyn wasn't alive but a couple minutes when the nurses and attending folks informed me she would have to be taken off to the Neo-natal Intensive Care Unit (NICU).
I follow Kaitlyn from the birthing room to a private little room inside of the dark and quiet NICU. I had to ask if I could hold her for a minute before they started hooking up leads and monitors. Begrudgingly, they agreed.
Thankfully, I was allowed a couple minutes before gently handing my baby off to others. I type this more than a week later and it still makes me sad to think I had to hand her to anyone but Kristi.
The first few hours after the birth consist of me escorting family members back to see Kaitlyn. We can only have two people in "The Unit" at a time. Throughout all the trips back and forth the nurses, and there were at least five that I saw, were trying to find a vein in Kaitlyn to administer IV fluids. Poking, and poking, and poking. Hands, legs, feet, arms. With every family member it's a new nurse trying a new spot. Sandy leaves the room. Barbara looks away.
They cannot find a good vein yet because she doesn't have much fluid in her, and they cannot put fluid into her until they find a vein. So they poke my baby again. They don't want to put the IV into the vein in her head unless nothing else works; it's just too disturbing for parents and relatives to see.
Kristi comes to see the baby a few hours later. It's after 3 AM I think, maybe 4 AM. Finally the IV is in. Our baby is on a breathing machine, CPAP. She has an IV with Antibiotics and saline fluid with Dextrose. A light and sensor combination is wrapped around one foot to measure 02 levels in her blood. She has three leads attached to her chest. Another one attached to her stomach; this one under a little gold duckie.
The problem, the key problem, is our baby is breathing too fast. Instead of 40 times per minute she is panting at 100 times per minute. Think of how exhausting that would be. I'm told she doesn't need extra oxygen, not yet, but she needs the breathing machine to keep pressure in the lungs so they don't collapse. Her blood gases are a little off too, but not enough we need to worry about them now.
I get to bed about 5 AM and wake about five hours later. I slept through the doctor visit, again.
She's stable. She needs the pressure for her lungs, but not oxygen; this makes the nurses happy. Her blood gases are better. We cannot hold her, not while the CPAP is attached. The day becomes a blur.
 Saturday, Aug 19
Saturday, Aug 19Another late night, another late wake-up. Kristi doesn't feel good. Most ladies are told to walk around after giving birth (isn't that a funny phrase, "giving birth?"). Not Kristi; her blood pressure was 100 over 50 yesterday. It's still too low today. Instead of walking she has a wheelchair; without it, she would fall over.
We see the baby some. A few people stop by to visit, it's nice they could come by.
Kaitlyn is doing better. Blood gases are fine, the pressure in the CPAP has been reduced. Antibiotics and fluids are still being administered by IV in the foot. The culture they are growing to see if the antibiotics are even necessary is negative so far. We really aren't sure what the problem is.
The likeliest issue is that she didn't and cannot get rid of the fluid in her lungs. This will go away with time. The next likeliest issue is that her lungs are under-developed. This is seen as "probably not true" because she would be getting worse instead of better if it was true. The third potential problem is an infection, hence the use of antibiotics.
 Sunday, Aug 20
Sunday, Aug 20We were given the orders from Kristi's substitute doctor, we can check out and go home today. With a baby just downstairs it's a mixed blessing so the question is when will we actually leave. We've talked with our nurse, Yvonne and she said something like, "It's Sunday until midnight, you can leave when you want. Let me know when you want to leave. "
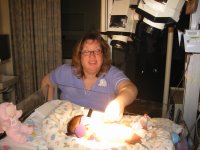
Kaitlyn is doing better, thank goodness. The culture is negative so far, so we can stop the use of antibiotics. Also, she's off the CPAP (breathing machine) and just on a nose canula. That's the little tube they put under the nose to give people oxygen. So yes, she did not need any oxygen yesterday when she was getting pressurized air, but today she does. I'm not sure why that would be, but you've got to trust the doctors. The great thing about this change in air supply is we get to hold her now.
As you can see from the picture, Kaitlyn is under a couple of bright spotlights and wearing purple shades. The lights are how babies get treated for high bilirubin, the stuff causing jaundice in babies. For us this is caused by a confluents of events; a liver that is not completely developed (common in all babies), bruising from the birthing process (fairly common in natural births), lack of bowel movements (caused by the use of an IV instead of regular feeding), and random chance.
We left the hospital around 6:30 PM. Kristi's not feeling well yet and we're going home to rest.
 Monday, Aug 21
Monday, Aug 21Kaitlyn is still subjected to the lights and a nose canula. She's getting better, they have reduced the amount of oxygen they're feeding her through the canula and today we start trying to feed with a bottle. She was fed formula yesterday, but because of all the tubes and sensors it was fed directly through a tube into her stomach.
We spend all afternoon in Kaitlyn's little room and late into the evening too. Kristi is tired and should be resting, but she wants to be here, with her baby.
For dinner we at with a support group for parents who have children in "The Unit." We heard the stories of a children who "graduated." I cried as I listed to a parent talk about the joy of her daughters and the pain she felt when other people looked aghast at pictures her tiny babies. The struggle to maintain her relationship with her husband and Herculean effort to support and nurture her children. How she celebrated all the tiny victories of her children's growth.
I know so little about this kind of suffering. My girl will be home in a few days not a few months, and this gives me an assurance they can only dream about. I am, we are, even in this time of less than perfectness, still blessed.
 Tuesday, Aug 22
Tuesday, Aug 22I really like this picture. The expression is so cute. You can imagine she is thinking so many things. A developmental expert might tell me she's practicing her muscles, but to me she's a beautiful and inquisitive girl exploring her world.
We're doing well; the doctor is very pleased with our progress. I asked the doctor to rate how serious Kaitlyn's condition was on a scale of 1 to 10, where 10 means it's a very serious situation for the NICU. The doctor said, "Let me answer a different question. How concerned am I about her? Zero. I have no concern that she won't get better and be healthy." Wow, isn't that great news?
Since we are doing so well, that means we can go home somewhere between two and five or more days. The key is she needs to maintain her progress and have no new or reoccuring issues come up for the next few days. We'll keep our fingers crossed.
 Wednesday, Aug 23
Wednesday, Aug 23Today we moved from The Unit to "Baby Steps." Baby Steps still requires people know the password to come visit our baby, but it means she is making lots of good progress. The big difference is that babies in the NICU are being monitored for their conditions, while over in Baby Steps the concern is maintenance and growth.
For us, this means we want Kaitlyn's bilirubin levels to decrease without use of lights or any other treatment. We also want her to continue to breath and maintain her heart without any problems occurring. Actually, it's okay if a problem occurs, it's that Kaitlyn needs to self-correct the problem within 20 seconds without any outside intervention.
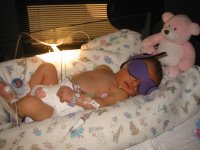
As the good doctor said to me yesterday, they tend to over-monitor babies and this just induces more concern than is warranted. Babies at home have the same kind of problems, but without all of the fancy monitors they recover on their own and parents don't go through the heart-wrenching feeling when the monitors start beeping. The picture above is Kristi looking at the monitor when it beeped a heart rate warning. It was actually just a monitor issue, but it's hard to stop looking up when it's beeping about your baby.
 Thursday, Aug 24
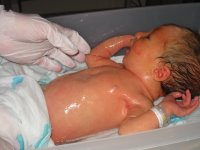
Thursday, Aug 24Maybe, just maybe, we can home tomorrow. We were told yesterday it would be Saturday at the latest, but this is getting better. In honor of the special potential the nurse suggested we give Kaitlyn a bath.
Everything went well with the bath and we only stayed at the hospital for a bit today (less than six hours). This is great because Kristi has not recuperated from the delivery yet. We're going to go home and get some extra rest. Not a lot of rest, but extra compared to what we've been getting lately.
 Friday, Aug 25
Friday, Aug 25We call into The Unit every few hours to see how our baby's doing. This morning when I called the nurse said, "She's doing great. The doctor hasn't written the orders yet, but you can take her home today."
I was so excited I almost told the nurse, "I love you."
We started getting ready to go to the hospital, but with the extra phone calls we started making it took a couple hours to get out the door.
Once at the hospital it took some time for the nurse and the doctor to get free enough to talk with us, but who cares? Really, we're going home today, why should we care about a few extra minutes?
And so ends our week in the hospital. And if you didn't know this already, you can click on the pictures above to see a larger version. Thank you all for your concern, thoughts, and prayers.
2 comments:
So happy to hear that things have gone well Jeffrey and Kristi. Both of our boys spent at least 7 days in the NICU and your post brough back vivid memories...particularly when you mentioned the little gold duckie on the temp sensor. It's a scary time but it certainly makes you appreciate everything that much more. I hope that everyone has continued to improve and that Kristi has been able to finally recover now that she hasn't had to spend all her time going back and forth to the hospital. Best wishes for Kaitlyn!
I'm so happy for the three of you and am glad that everything is okay and you have started life at home with Katie. Gage was in the Special Care Unit when he was born but only for about 36hrs I believe. He was with me in the post-natal ward the next night. You never stop worrying even if they just want to monitor their food intake.
She is a lovely little girl and I wish her and you & Kris all the best and a bright future for your little princess.
Post a Comment